Unmet Need
Postoperative clinical complications are a hidden pandemic affecting over 25% of patients undergoing major surgery.
310 million major surgeries are performed each year; of which 40 to 50 million in USA and 20 million in Europe. 26.8% of patients with major surgery experience postoperative complications. Increased duration of postoperative complications results in prolonged ICU- and hospital-length-of-stay and increased re-admissions to the hospital.

POSTOPERATIVE COMPLICATIONS AND HEMODYNAMIC INSTABILITY
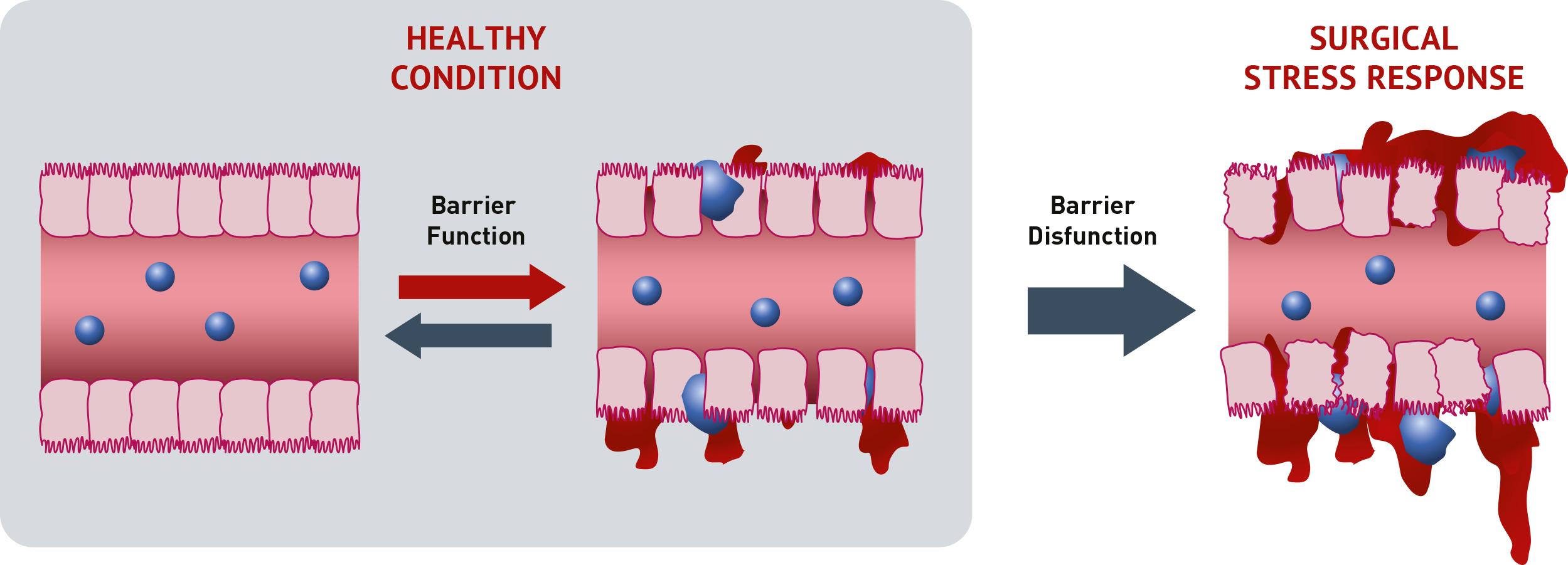
Major surgery induces a major vascular stress response. Throughout this stress response, barrier function and permeability of microvascular walls is affected, causing capillary leakage with extravasation of blood cells and fluids that hamper healing of postoperative complications. The microvasculature regulates exchange of oxygen, nutrients, and immune cells to tissues – and dysfunction of that exchange causes reduced resolve of postoperative complications in those tissues.
Current Treatment
Standard of Care includes administration of intravenous fluids to maintain hemodynamic stability but can paradoxically worsen the duration of postoperative complications.
Fluid administration is a delicate balance: too little can lead to tissue hypoperfusion and damage, while fluid overload can cause tissue oedema and further increase postoperative complications and hospital length-of-stay.
There is currently no therapy available to distinctly moderate microvascular consequences of surgical stress, with or without fluid therapy. Reduced use of fluid does not reduce the length-of-stay but significantly increases hospital morbidity instead.
The focus needs to shift to reducing the capillary leakage rather than to add fluid. With millions of patients suffering from postoperative complications each year, there is a significant unmet medical need for fast-acting drugs that target capillary leakage to maintain hemodynamic stability.
EBI’s Promising Solution
EA-230 presents a novel and promising solution to improve hemodynamic stability and reduce duration of postoperative complications after surgery. EA-230 additionally presents attractive options for use in many other market segments associated with acute tissue injury, such as non-surgical trauma, radiation, burns and acute systemic inflammation, each with additional potential market value.

